Australasian Diabetes Advancements and Technologies Summit
ADATS
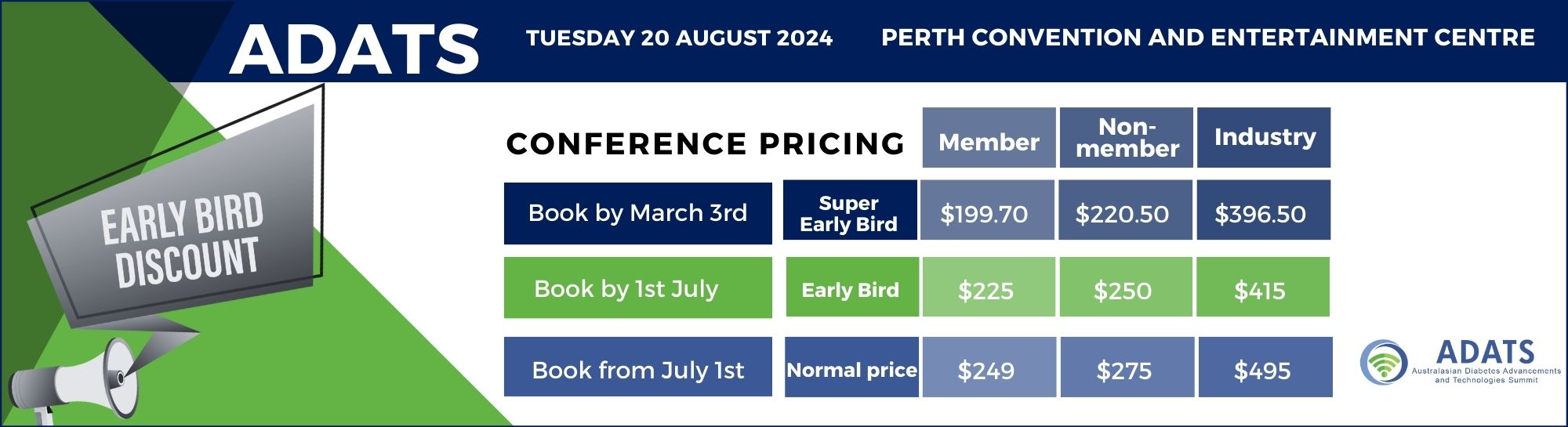
The highly anticipated 8th annual Australasian Diabetes Advancements and Technologies Summit (ADATS) will be hosted at the Perth Convention & Exhibition Centre on Tuesday, August 20th! This year, ADATS returns, once again preceding the Australian Diabetes Congress at the Perth Convention Centre.
Prepare for an exhilarating day filled with renowned international speakers and leading experts from Australia, as we delve into the future of diabetes technologies and cutting-edge therapeutics, both locally and globally.
Whether you’re a newcomer to diabetes care or a seasoned professional, this event offers something valuable for all those dedicated to enhancing the lives of individuals with diabetes.
NOTE: Registration to ADATS is via the Australasian Diabetes Congress (ADC) registration page. You can register for ADATS without registering for ADC or do both at the same time.
If you require further assistance with registering for ADATS2024, please feel free to email Lei or Marj at admin@nadc.net.au

Watch ADATS full presentations on your computer, tablet, or smartphone at your own pace.
AUSTRALASIAN DIABETES ADVANCEMENTS & TECHNOLOGIES SUMMIT (ADATS)
The main topics that are discussed at ADATS include:
- What’s new in Diabetes Technology
- The complexities, intricacies, and disparities of diabetes technology
- Quick bytes Session

I would like to receive updates on ADATS 2024


ADATS registrants will be provided with a detailed certificate of attendance that can be used as evidence of continuing professional development.
MEET THE ADATS 2021 SPEAKERS
SESSION 1: Virtual Care and Diabetes –the lived experience, research and the future

DR KOREY HOOD
Time: 10:45-11:05
Topic: Leveraging telehealth and digital tools to optimize use of diabetes devices

A/PROF ANTHONY RUSSELL
Time: 11:05-11:25
Topic: Using technology to improve the level of care for people with diabetes in rural areas

A/PROF GLYNIS ROSS
Time: 11:25-11:45
Topic: What do we need to develop/improve with the technology that we are using today
SESSION 2: Data, Quality & Best Practice in Diabetes Care and Technology

DR ELAINE PRETORIUS
Time: 1:10-1:30
Topic: Diabetes Technology Standards & Accreditation

DR WILLIAM POLONSKY
Time: 1:30-1:50
Topic: Impact of PROs (Patient Reported Outcomes) on adult clinical care: why, when and how?

MARGARET LOH
Time: 1:50-2:10
Topic: Automated Insulin Delivery—Best practices for onboarding and follow-up

A/PROF JANE HOLMES-WALKER
Time: 2:10-2:30
Topic: Real world data vs reality: Strategies for improvement of metabolic control in adults with T1D
SESSION 3: Emergencies, Complications and Innovation

DR RAHUL BARMANRAY
Time: 3:20-3:40
Topic: In-hospital Glucose Emergencies in a Digital World

A/PROF ROGER CHEN
Time: 3:40-4:00
Topic: 100 years of Insulin; where we are now and what’s ahead

JASMINE SCHIPP
Time: 4:00-4:20
Topic: How Adults with Type 1 Diabetes Are Navigating the Challenges of Open-Source Artificial Pancreas Systems

PROF JONATHAN GOLLEDGE
Time: 4:20-4:40
Topic: Technologies to enhance accuracy of at risk foot assessment
ADATS PROGRAM

PAST ADATS
ADATS was launched for healthcare professionals in Australia in 2017, to provide an access to the latest information on diabetes advancements and technologies. The event is the result of the commitment by the NADC to improve the knowledge and skills of healthcare professionals in Australia. ADATS brings together world-leading experts, academics and clinicians with a shared focus and passion in advanced technologies and therapeutics in diabetes.
The event is the result of the commitment of the NADC to improve the knowledge and skills of healthcare professionals in Australia in the area of diabetes and technology.